 |
| "Get Well" flowers |
It was a Mayday call on a Monday May Day morning that brought about the ambulance ride, through peak hour traffic, to a major city hospital.
The ambulance officers were absolutely lovely–calm, kind and professional–as they always are when taking me with them.
There was no argument this time. There was something about their observations that they didn't like the look of, so they packed me up and off we went on that chilly, autumn morning.
Connective tissue disease (MCTD) / Lupus (SLE) causes lots of aches and pains.
I've experienced all sorts over the years, including chest pains.
The first ones caught me when I was as young as 12 years of age. The pains are usually momentary but even so, they can literally 'take my breath away'. Explanations for previous episodes include pleurisy and scarring on the lungs presumably from severe childhood asthma.
These days, I like to think I am well-practised in identifying the types and causes of the pains. They are usually benign and my typical response is to stop and wait until they disappear–they always do; except on this Monday morning.
Monday's pain took me by surprise and had a different quality in comparison to past sensations. It was quite disconcerting when it worsened with activity and persisted despite rest. Soon it began to spread so the ambulance was called.
When living with chronic illness, it is important to know how to manage it and when to get help. I've had arrhythmias and heart flutters in the past so my standing orders are to call the ambulance whenever I get chest pain. (In practice, I don't always call the ambulance–if I rang them every time there was a bit of pain, I'd never get away from the hospital–so far, so good; please don't tell my GP!)
Of course, an ambulance call is never undertaken lightly. With MCTD and SLE, my doctor's main concern is a complication called pericarditis (inflammation of the membrane around the heart). Lupus can cause a number of complications which can damage and weaken the heart.
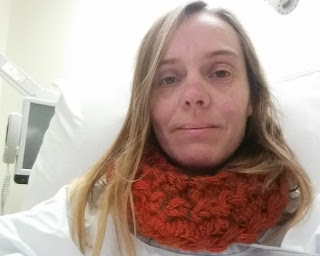 |
| In the emergency department it's all okay because I'm still wearing my hairpin crochet cowl to keep my neck and shoulders toasty warm. Thank you to Catherine R. for giving me the courage to share pictures even when I'm not at my best–this is the reality of chronic illness. |
on Monday, 1 May, the electrocardiograph (ECG/EKG) readout was inconclusive, suspicious and in need of further investigation.
Luckily, I was all rugged up from doing the 'school run' early that morning and I am glad I had my woollens with me because the hospital gowns are not warm at all! I refused to remove my cowl.
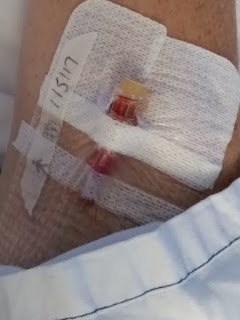 |
| Emergency department procedure no. 1: insert IV cannula now while veins are still good. Convenient and time-saving in an emergency. |
This little cannula gadget is a great little invention for administering intravenous fluids and medication etc. It can also be used to take blood samples. You can even 'piggy back' an extra port (like a double adapter) which allows the drip contents to go into one and an injection of medication into the other but all going into the same vein at once (only one puncture).
I was thinking to myself how convenient it is nowadays to have one needle for all of those jobs instead of receiving multiple jabs in multiple places like it used to be when I was a child.
 |
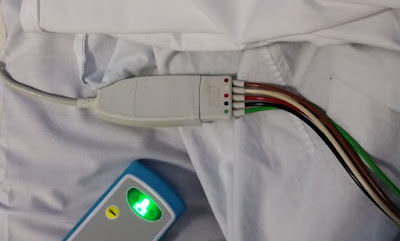
| The view from the scarf as I get plugged into the heart monitor. (Emergency department procedure no. 2.) |
Cannulas can be a higher risk for infection and I think that's why the nurses like to minimise the use of it. It is important to replace the cannula every three days to prevent infection. (That's my understanding of it anyway. Any nurses out there are welcome to correct me if I am wrong.)
Meanwhile, my vital signs were being measured as I was being hooked up to a different heart monitor. This involved the application of new electrodes, informally called 'sticky dots'–essentially square stickers with a conductive sticky gel on one side to stick to the skin and, on the other side, a metal knob to which a lead can be clipped in order to send the signal to the heart monitor machine. Boy! Are those dots sticky!
The previous 'dots' from the ambulance needed to come off to make way for the new ones. Like removal of band-aids / sticking plasters I highly recommend the 'quick-rip' method! 1-2-3-rip! Phew!
The next three days were spent hooked up to a heart monitor and undergoing various tests including more complicated ECGs where more leads were added, not just to my torso but to my arms and legs too! Along with that came more ripping off of existing sticky dots because they were in the way of the precise positioning of the complicated ones.
I can't imagine how bad this would be for hairy-chested men to have so many sticky dots on and off all the time. Ouch! I wonder whether the nurses bother to shave the area before applying the dots.
When I said those babies were sticky, I wasn't joking. In the past, I've rarely had troubles removing them. The stickiness left behind is similar to the glue residue of a band aid that's been on for a while. Usually it dissolves easily and falls off as soon as you apply warm water and a bit of soap; no problem; but these heart monitor stickies were nasty. They took days to wash off. I almost gave my skin welts from the friction of rubbing the spots so hard with the face washer (and that was two days later)! It is two weeks since the sticky dots were removed and the square marks can still be seen on my skin!
I soon became well-acquainted with my constant companion, the spaghetti tangle of leads, which I soon learned to keep organised but it was annoying at night. I had a habit of turning over in my sleep and unconsciously disconnecting one or more of the leads, at which point an alarm would go off. Bye, bye, sleep!
The most annoying thing at first was needing nurse assistance to disconnect me and reconnect me whenever I needed to leave the bed for the bathroom or when the alarm sounded. I was getting very frustrated with it all so I soon learned how to do it myself. If one lead came undone, I worked out how to clip it back on but two or more had me a bit flummoxed until one of the nurses taught me a little story to remember which colour lead goes to which dot:
White on the right (on the patient's right hand side)
Green grass on the ground (below the white)
Smoke (black) is found above fire (red)
Leaving the brown one to go in the middle.
My drawing is an approximation of the sticky dot positions. If I needed to stick the actual dots onto someone precisely, I would have no idea about how to do that to make sure it is in the right place but at least I no longer needed someone else to help me fix a loose lead. (I'm a very independent patient!)
Some people don't seem to mind being in hospital. They talk about it like a holiday break using the mindset of "no housework, breakfast in bed etc." but that is definitely not me!
Give me my own bed anytime. Fortunately, my family were able to bring in some essential comforts from home.
 |
| Boomerang pillow Thank goodness for small comforts from home! |
These are the essential things that make time in hospital bearable:
- boomerang pillow to support myself sitting up and for sleep. It was particularly useful one noisy night because it meant I had two pillows–one to rest my head upon and one to cover my ears!
- transistor radio with earplug–the level volume of radio transmissions is good for screening ambient noises and the newsy programs keep me in touch with the happenings of the outside world
- mobile phone for keeping in touch with friends and family and for using the library's eBook and audioBook service. One can 'borrow' books remotely using a phone app without having to worry about fines for overdue returns because the app automatically 'returns' the file when the borrowing period has expired.
- my own food. It astounds me that after decades and decades, hospitals in this country still cannot cater for special diets. For three whole days I was served meals that I couldn't eat even though the staff knew I could not tolerate those foods! Luckily I had some home cooked leftovers in the freezer etc. which my family brought in for me.
For those of you who like to indulge in coffee and tea, scroll down quickly and look away NOW unless you want to be horrified by the next picture!
 |
| Caffeine was not allowed. This sign was placed next to my bed. Chocolate was also banned. |
Lupus and MCTD come under the arthritic umbrella. A common adage with arthritis is "use it or lose it". Maintaining mobility is important to prevent joints from stiffening, and to maintain strength and fitness. The combination of inactivity and an uncomfortable bed left my body desperate for some decent physiotherapy.
The other rule was no caffeine because it messes with the heart readings and test results. That meant no tea, coffee, milo, chocolate etc.
The big bedside sign was annoying because the aftenoon tea trolley would come around offering everyone a cuppa with a snack such as biscuits, cake or fruit. The tea trolley people would see my sign and stroll right by, not realising that I could still eat an afternoon tea snack despite not being able to have their drinks.
I don't eat biscuits and cake but after getting useless meal trays, I was hungry and desperate for something healthy like a banana or apple. (Ironically, hospital food is not healthy.) I had to be alert to catch the trolley before I missed it. On the first afternoon, that particular trolley lady argued with me because she was convinced that she was not allowed to give me anything because of the 'no tea' sign. She reluctantly let me take a banana, mumbling,"I shouldn't be doing this."
 |
| Oops! Jodie died …of boredom! |
So there you go…stealing from the tea trolley…cheap thrills for bored little me.
"Why were you bored,
pray tell?"
pray tell?"
I hear you ask,
"Did you not have any crochet
with you?"
Oh yes! I had been working on a broomstick crochet cowl but it was finished as far as I could go on the first day so I had to wait until my family could bring in something else to crochet.
When I get bored, I get mischievous, hence the flatlining on the monitor! Don't you love the question mark?
 |
| There's a 'stripe thing going on' –stripes in the scarf and stripes created by the coloured leads. Perhaps this picture will inspire a stripey project or colour scheme. |
Besides all the spaghettis and sticky dots, I went for a ride down to the nuclear medicine department for scans and that is where the IV cannula was used to inject radioactive material into my system to see what shows up on the PET scanner. Positron Emission Tomography. That's one I've never had before. Sorry I couldn't take photos there.
I'm always impressed by the capabilities of technology these days; these machines that can see inside us without having to open us up. There once was a time when the only way people knew how to find out what was happening inside was to open someone up. I'm grateful I don't live in those times.
It made me think about the amazing tech I have already seen and it truly is fascinating, albeit a bit of a worry to have experienced so much of it firsthand as a patient. Like Pat Benatar's notches on her lipstick case*, I tried to remember how many different scans or procedures I've had and, honestly, I lost count and forgot so I continued to lay still and tried to work out what I would put notches on, instead of a lipstick case, for all those encounters with imaging technology.
I was also grateful that the PET scanner was not as uncomfortable as the CT scanner or the MRI machine. (Computerised Tomography and Magnetic Resonance Imaging)
 |
| This time Jodie's really gone … … home, that is! Hooray! |
By the end of three days, I had made friends with the other people in my ward bay and it was funny to be referred to as "our young lady"by the other patients.
"Young!?"
I wouldn't say I was that young anymore but I didn't mind the sound of that word after my body has been feeling so old lately.
I suppose it was the cardiac ward, and most of the people with heart problems were much, much older than me, as one would expect.
When all the test results came back, I was allowed to go home. Hooray!
No sign of a heart attack, no major heart damage done, no immediate emergency so I was free to go.
Although the cardiologist could tell me what I didn't have wrong with me, he could not tell me the cause of the original pain so it looks like I will be back on the rheumatology roundabout again.
You would think that after taking so much blood, the hospital doctors would also be doing rheumatology studies with it (which I thought the emergency doctor had mentioned), but no, they only took cardiology tests. It is frustrating when doctors put patients into little boxes and can't or won't look outside that box. Someone at the hospital described specialists as "knowing more and more about less and less" as their specialties become more narrowly focussed and increasingly specialised.
Nevertheless! There's nothing so urgent than to get disconnected and unplugged, cannulas removed etc. and bag packed as when the doctors say you can be discharged from hospital.
Let's go!
Here's the happy ending to this chapter …
 |
| A pretty posy from a dear friend greeted me on my arrival home from hospital. |
* "Hit Me With Your Best Shot" hit song from the 80s by Pat Benatar
P.S. I worked out another acronym for MCTD after this experience and, on 3 May, added it to the comments in the blog post about the New MCTD Resource Page (5 October 2014).
Links & References
Life in the Fast Lane, web site, Australia / New Zealand:
- Burns, Edward, "The ST Segment", updated 17 April 2017: https://lifeinthefastlane.com/ecg-library/st-segment/
- Nickson, Chris, "Pericarditis", updated 2 April 2017: https://lifeinthefastlane.com/ecg-library/basics/pericarditis/
Lockshin, Michael, MD, "About Lupus: Caring for your Cardiovascular System", Lupus Research Alliance, formerly S.L.E. Lupus Foundation, 275 Madison Avenue, 10th floor, New York, USA, web page accessed 15 May 2017: http://www.lupusny.org/about-lupus/fight-lupus-body-and-mind/caring-your-cardiovascular-system
Lupey Loops blog, Australia:
- "Broomstick Rainbow Finished for You", 10 June 2017: http://lupeyloops.blogspot.com.au/2017/06/broomstick-rainbow-finished-for-you.html
- "Lost Without Lists", 2 September 2015: http://lupeyloops.blogspot.com.au/2015/09/lost-without-lists.html
- "Packing for Hospital", 7 December 2014: http://lupeyloops.blogspot.com.au/2014/12/packing-for-hospital.html
- "New MCTD Resource Page", 5 October 2014: http://lupeyloops.blogspot.com.au/2014/10/new-mctd-resource-page.html
National Resource Centre on Lupus, "How Lupus Affects the Heart and Circulation", Lupus Foundation of America, USA, medically reviewed 11 August 2013, accessed 15 May 2017: http://www.resources.lupus.org/entry/heart-and-circulation
Richardson, Catherine, Finding My Miracle: tackling chronic illness with joy and humour, one day at a time, blog, Canada, 2014–2017: https://findingmymiracle.com/


Gosh. Jodie I'm glad you got back out of hospital. You stay so positive and it inspires me to try not to grumble. I'm so pleased you had your crochet with you!
ReplyDeleteYou are allowed to grumble, Tamara! Sometimes having a grumble helps to get the negativity out of the system and that's healthier than bottling it all up.
DeleteAt the same time, there are lots of things to remain positive about and I choose to focus on those most of the time. I feel so lucky to live where I live, to have access to health care, medical expertise and a supportive environment. Any day where I'm not bedridden is a good day and I rejoice in that.
I must admit to having an element of 'ignorance is bliss' as well, taking each day as it comes, trying to make the most of it because you never know what tomorrow may bring.
Having said all that, I did have a 'down day' yesterday as I reflected on what this all means, hearing my doctors words in my head, being reminded to take my condition more seriously (of course I do take it seriously anyway but maybe I need to be more mindful) in the sense that although I can't see it, this illness can be doing silent damage which can culminate in an emergency; so while I can be feeling relatively well and mobile, I still need to be careful and take it easy. It's really hard to find a balance and to reign in my enthusiasm, passion and gung-ho attitude to life! (I have a feeling you can relate to that.)
Back on a positive note, sitting around gave me the chance to get the scarf crocheted once and for all, ready to take home and block before finishing. This one will go to Gallery M.
Thank you for your support. xx
Oh my what a week you had! I am very happy to read you are now out of hospital! Plus I am glad you have such a good support network (wish I could pop in!) and got your own food! I hate hospital food - makes me feel even sicker!
ReplyDeleteTake care
Anne
I wish you could pop in too, Anne. I can see us sitting there together with our crochet hooks and sharing stories.
DeleteThe hospital food here is dreadful. Processed muck with additives, preservatives, colours etc. that make me sick. It is crazy. Hospitals are not really the best environment for healing!
Celebrity chef Jamie Oliver did a crusade to overhaul the British school lunch system. We need someone here to overhaul the health department food. One man I met in the hospital lost so much weight because he refused to eat the meals and that upset his other health conditions. Honestly, I don't understand why health departments cannot join the dots.
I always leave hospital in worse condition than when I went in. It's not right.
The more we stay away from hospitals the better!
I hope you are going well, recovering from your recent travel and that the jolt back to reality after a holiday season isn't too hard! Take care xx
Note to myself - add emergency knitting to the hospital bag! What on earth was I thinking of?
ReplyDeleteWhat *were* you thinking of, Cat? (Shaking my head, tut-tutting!)
DeleteHahaha Emergency craft supplies are essential for calming the nerves and staying sane. Glad to be of service! ;-)
PS If it was the RAH you were in and it happens again then send me an SOS and I'll pop the trike on the train and bring you some crochet - seriously!
ReplyDeleteYou are such a sweetheart, Cat! I will remember that.
DeleteI had a phone call with my daughter that first night as she went ploughing through my box of WIPs. It was funny because I didn't realise how many things I had there as she's describing one discovery after another. Each project is kept in its own bag so it was relatively easy to find something to bring in - it was the choosing that was difficult!
There are easier ways to get projects done than by being in hospital so I hope to steer clear of the RAH or any of them for a while. Your support and offer of help is much appreciated. xx
Wow - epic post for an epic experience, Jodie! So glad you're home again, and frustrated on your behalf that you didn't leave with something conclusive. It's all too often the way, though, isn't it with these diseases?
ReplyDeleteOh - and DON'T get me started on hospital food. It's just not that hard to make simple, nutritious food that tastes reasonable! If thousands of businesses who have to put out bulk food for mealtimes can do it, the hospitals ought to be able to. I have several strategies for dealing with it - thankfully haven't had to put them into play for any lengthy stays for a few years now.
DeleteYou are so right about the food, Kaz. I totally agree. The doctor asked me what I could eat and I told him: fresh vegetables and basic foods, without all the sauces (with their additives). He agreed that it shouldn't be too hard to serve basics like that.
DeleteI have a lactose-free (LF) diet so the hospital brought me soy milk but I don't drink that either because soy is a phyto-oestrogen and I don't need to feed the endometriosis with any more oestrogens of any kind.
My family brought in a carton of LF-milk and some LF-yoghourts, fresh fruit and wholemeal bread. The hospital serves either white bread (which I don't digest very well) or multi-grain bread (which contains rye, one of my allergens) so hospital bread is useless.
One of the nurses stole some spreads from the staff kitchen and, at mealtimes, I stashed away the un-used cutlery so I would have something with which to spread my bread whenever I felt like it!
On TV last night there was a program called "War on Waste" which showed how much fruit and vegetables farmers had to throw out because the supermarkets would only accept the 'perfect' specimens. Why can't that nutritionally perfect 'imperfect' produce be distributed to hospitals to be used there?
Then the health service can't complain that fresh food costs too much - this was food being discarded and wasted.
There's a bit of 'chicken and egg. thinking too. I've heard the excuse that the health service doesn't want to spend money on expensive food because much of it doesn't get eaten and therefore would be a waste of money! Ummm...maybe if the food was palatable and healthy, people would eat it?
Yes, Kaz, we are of the same mind "Don't get me started!" hehehehe Surely it's not that hard? It's not re-inventing the wheel. There was a celebrity chef, who's name escapes me, in the eastern states who was on a hospital food crusade but I wonder if he has run up against a bureaucratic brick wall because I haven't heard anything of the idea for a few years now.
Wouldn't it be good if people could wake up and fix it soon? Perhaps instead of cards and flowers, we should bring fresh food to our hospitalised loved ones.
Thanks, Kaz, for reassuring me that I am not weird in wanting 'proper food'. May you never need to put your hospital food strategies into action.
I hope this finds you on a relatively good day and that your pain eases. xx
You've really been through it, Jodie, I'm glad to hear that you are back home. A big hug!
ReplyDeleteAmalia
xo
Aw, thanks for the big hug, Amalia! I am a 'huggy' person. That's lovely! It is a comfort to receive your well wishes. I'm breathing a sigh of relief to be home and back to my own routines.
DeleteAnnoyingly, the hospital didn't serve breakfast until 8 - 8:30 a.m. The advantage of having a secret stash of breakfast foods, meant that breakfast and medication could be taken early.
I prefer to be an early bird (it's the best part of the day) whenever the body is agreeable. Are you an early or late riser, Amalia?
Hugs in return xxx
Jodie! Hope you're better now. Not nice when this happens. I'm sitting through a slight myasthenia flair for a couple of weeks now, but weaned off to kiddy dose. Still, it's an irritation (thankful that it's just an irritation!). Plus a bad head cold, so today, I'm on the couch, doing nothing and nothing and nothing more.
ReplyDeleteAll the best!
That's sad news, Stel, and frustrating for you too surely because you are such an active person. Strong medications that require weaning are a hassle. I hope the side effects (if any) aren't too horrendous.
DeleteDo you think your head cold triggered the latest flare? I want to march over there and tell your head cold where to go!
I hope you are as comfortable as you can be under the circumstances and you aren't going too crazy doing nothing, even if doing nothing is the best thing to do right now.
May this reply find you feeling a little better and on the mend.
Here's a corny medical joke to make you smile (or groan or both):
Patient: Doctor, Doctor! I'm sick of hanging around like a set of curtains.
Doctor: Sit right down and pull yourself together!
(I can hear the face-palms now)
Keep smiling, Stel. Take it easy and get well soon. xxx
I was fretting and fretting as I read through your post but then the line...
ReplyDeleteJodie died... of boredom....and I laughed out loud.
That's the spirit.
I am glad you had your crochet with you and good on you for not taking off that cowl. It looks fabulous.
Thank you for your recent comments on my blog. I appreciate hearing from you and especially your comment on my post about the writer's group. Don't worry about me - I am doing better - meditating, increasing meds and I am going to a new support group tonight. We are all ok. You are ok. I am ok. Life goes on.
Oh Mary Anne! I am so sorry for worrying you! That certainly was not my intention. Please accept my apology! I'm so thankful you were able to have a laugh. I don't want to leave you feeling anxious.
DeleteThe idea of this blog entry was to let everyone know what was happening with me, especially since there weren't any new blog entries for a while. (The original blogging goal was to have at least one new entry per fortnight.)
Even my local friends use Lupey Loops as a way to 'check-in' to see what I've been up to. By posting the news here, it saves my energy because I don't need to re-tell the story too many times.
I also wanted to reflect upon the experience and remember details for myself. The blog is a handy space for keeping such thoughts and if people find it interesting, learn something or feel less alone in their similar experiences, then that's a positive thing.
Thank you for your sweet compliment on my scarf. Did I blog that one? I can't remember! If not, I must put it on the blog list.
I'm sorry my comments on your blog always seem belated. I get so busy for a time and then I will do a great big catch-up with everyone all at once. I usually manage to regularly read blogs on my phone but I have trouble leaving comments from my phone so the comments get left for the 'catch-up' time when I can sit at the computer.
I wonder how you went at the new support group. Even when we want to do new things with new people, it can still be out of one's comfort zone. I hope this new group of people were able to put you at ease and actually do what they are supposed to do - support you.
Love your last line - the rhythm of it. Life is ok. xx
Here's the deal. No apologies necessary for anything. I love getting a spate of comments from you - it is like we are catching up over tea (or something stronger). I didn't make it to the support group this week because of a nasty headache, but I am meditating everyday and it is helping.
DeleteHow did I miss this? It never popped up on my feed and now I am frantic because you must think I wan not thinking about you! I am so sorry I missed this and I am so glad getting to the end of it all that you are okay. You must think of me as a sorry friend and I apologize. Your health and well being are so important to me. I so wish you did not have to go through all of this but am glad you are better.
ReplyDeleteYou missed this in the same way that I missed your response a month ago! Sometimes our computer systems can be unreliable. Regardless, let me assure you that at no time did I ever sit down and think less of you due to a lack of a comment here. Banish the idea.
DeleteJust because there is no comment, doesn't mean that a person hasn't read the blog entry. It is understandable that it isn't always possible to leave a comment. My silly phone is a case in point.
This year, I've made a concerted effort to get to know the features on my 'smart'phone and it has been very handy, providing opportunities to read blogs in those spare moments here and there while out and about. The only problem with that is my naughty phone wants to 'correct' MY words and replace them with ITS OWN words when I'm not looking. I can check the writing before hitting the 'send' key and by the time it is posted, I see an abundance of 'corrections' that must have clicked through in the blink of an eye.
After too many embarrassing moments, I decided not to reply to blogs on my phone and remain self-disciplined in keeping to my computer keyboard for more accurate responses, even if they are a little late in coming.
So all those words from me, just to say, "Thank you for thinking of me, Meredith"
"No worries"! xxx